
Diagnosis And Treatment Of Knee Meniscus Tears
Meniscal tears are a common knee injury in both the sporting and the ageing populations. This injury has been linked to a 4-time increase in long-term risk of knee osteoarthritis (OA), so managing it well is important. Being able to correctly identify the risk factors that can lead to a meniscal tear can help with diagnosis, effective management, and the prevention of knee OA.
Knowing and improving “modifiable risk factors” (i.e. things we can change that affect your risk) for meniscal injuries plus early examination & treatment is key to avoiding potentially unnecessary surgical intervention. This is important because meniscal surgery has been shown to make patients more susceptible to degenerative disease (OA) later in life.
What Is The Function Of The Meniscus?
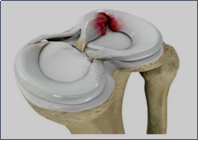
The meniscus has several important roles including:
· Shock absorption & re-distribution of forces throughout the knee joint
· Limiting the extreme ranges of flexion & extension
· Improving knee joint stability
In a mature meniscus the outer zone has a good blood supply however the inner zone has no blood supply. This significantly affects the ability of the meniscus to heal following a tear.
How Do Meniscus Tears Happen?
Acute meniscus tears typically occur when the foot is planted on the ground & a twisting movement happens through the knee, putting a shearing force through the meniscus. Degenerative tears are mostly seen in the middle to older aged population, whose normal daily activities can place more stress on the meniscus than it is able to bear. This can represent the early stages of knee OA.
Who Is At Risk Of A Torn Meniscus?
Acute meniscal tears can occur in both younger & older populations, usually due to a sporting injury involving twisting while weightbearing. Some sports with higher incidences of meniscal injuries include netball, soccer, basketball & rugby.
Degenerative meniscal tears are more common in the older population, & can occur more frequently with normal daily activities. The risk factors for a degenerative meniscal tear include:
· > 60 years of age
· Being male
· Higher BMI
· Occupation-related squatting & kneeling
Diagnosing a Meniscus Tear
There are several key indicators in a client’s history & physical exam to suggest a meniscus tear;
1. Localised pain on palpation of the knee joint line (i.e. localised pain to push on the joint line)
2. Pain or locking with end-range flexion (bending) or extension (straightening) of the knee
3. Mechanical derangement symptoms: locking, catching, clicking, or giving way sensations
4. Positive Thessaly test: the client stands on the injured leg while holding onto a bench for support. While the knee is in 20 degrees of flexion, they rotate their body internally & externally on the weightbearing knee. The test is positive if it reproduces the client’s symptoms
5. Swelling: A small-moderate swelling can develop 24-48 hours following an acute meniscus tear
Physiotherapy Vs Surgery For Meniscal Tears?
A solid body of evidence (see references below) over the last decade shows that conservative (physiotherapy) management is equally as effective as surgical management for meniscal injuries, plus it has less risk of increased future OA compared to surgical intervention. It has also been shown that delaying surgery while trying conservative treatment does not adversely affect outcomes.
So How Should We Manage Knee Meniscal Tears?

What these findings mean is that the recommended management pathway for meniscal injuries is an initial course of physiotherapy for 8-12 weeks, and only progression to surgical intervention if this fails. And even in these cases, pre-operatively building strength and stability provides significant benefits if surgery is later required.
How Can Physiotherapists Treat Meniscal Tears?
Physiotherapy focuses on exercises to rebuild strength & stability throughout the knee & the whole lower limb. We use proprioception retraining & strength exercises to restore knee control, stability, strength & function. Graded exposure to heavier loads are prescribed where appropriate, eg for a safe return to sport.
Manual therapy may be used to restore ROM and for pain relief where appropriate, however the foundation of effective management is exercise. By maximising knee strength and control we optimise knee biomechanics, function and resilience.
References
1. Lee, D., et al. (2018). Arthroscopic meniscal surgery versus conservative management in patients aged 40 years & older: A meta-analysis. Archives of Orthopaedic & Trauma Surgery, 138(12), 1731-1739.
2. Khan, M., et al (2014). Arthroscopic surgery for degenerative tears of the meniscus: A systematic review and meta-analysis. Canadian Medical Association Journal, 186(14), 1057-1064.
3. Mordecai, S. C. (2014). Treatment of meniscal tears: An evidence based approach. World Journal of Orthopedics, 5(3), 233.
4. Rathleff, C. R., et al. (2013). Successful conservative treatment of patients with MRI-verified meniscal lesions. Knee Surgery, Sports Traumatology, Arthroscopy, 23(1), 178-183.
5. Nepple, J. et al (2012). Meniscal repair outcomes at greater than five years. The Journal of Bone & Joint Surgery-American Volume, 94(24), 2222-2227.
6. Roos, H., et al (1998). Knee osteoarthritis after meniscectomy: Prevalence of radiographic changes after twenty-one years, compared with matched controls. Arthritis & Rheumatism, 41(4), 687-693.
7. Rogers, M., et al (2019). A cost-effectiveness analysis of isolated Meniscal repair versus partial meniscectomy for red-red zone, vertical Meniscal tears in the young adult. Arthroscopy: The Journal of Arthroscopic & Related Surgery, 35(12), 3280-3286.

